Section iv endocrine & reproductive physiology – The Thyroid Gland
Introduction
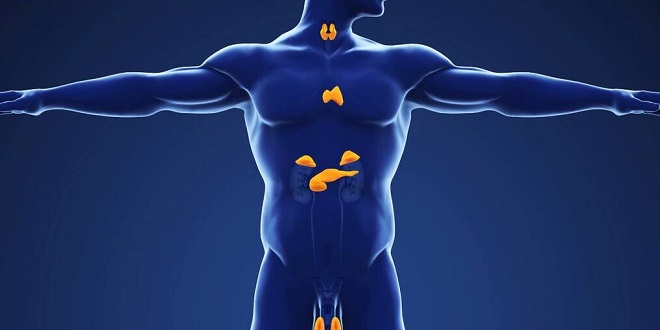
The thyroid gland is one of the larger endocrine glands of the body. The gland has two primary functions. The first is to secrete the thyroid hormones, which maintain the level of metabolism in the tissues that is optimal for their normal function. Thyroid hormones stimulate O2 consumption by most of the cells in the body, help regulate lipid and carbohydrate metabolism, and thereby influence body mass and mentation. Consequences of thyroid gland dysfunction depend on the life stage at which they occur. The thyroid is not essential for life, but its absence or hypofunction during fetal and neonatal life results in severe mental retardation and dwarfism. In adults, hypothyroidism is accompanied by mental and physical slowing and poor resistance to cold.
Anatomic considerations
The thyroid is a butterfly-shaped gland that straddles the trachea in the front of the neck. It develops from an evagination of the floor of the pharynx, and a thyroglossal duct marking the path of the thyroid from the tongue to the neck sometimes persists in the adult. The two lobes of the human thyroid are connected by a bridge of tissue, the thyroid isthmus, and there is sometimes a pyramidal lobe arising from the isthmus in front of the larynx. The gland is well vascularized, and the thyroid has one of the highest rates of blood flow per gram of tissue of any organ in the body.
Iodine homeostasis
Iodine is an essential raw material for thyroid hormone synthesis. Dietary iodide is absorbed by the intestine and enters the circulation; its subsequent fate is summarized. The minimum daily iodine intake that will maintain normal thyroid function is 150 μg in adults. In most developed countries, supplementation of table salt means that the average dietary intake is approximately 500 μg/d. The principal organs that take up circulating I– are the thyroid, which uses it to make thyroid hormones, and the kidneys, which excrete it in the urine. About 120 μg/d enter the thyroid at normal rates of thyroid hormone synthesis and secretion. The thyroid secretes 80 μg/d in the form of T3 and T4, while 40 μg/d diffuses back into the extracellular fluid (ECF). Circulating T3 and T4 are metabolized in the liver and other tissues, with the release of a further 60 μg of I– per day into the ECF.
Thyroid hormone synthesis & secretion
At the interface between the thyrocyte and the colloid, iodide undergoes a process referred to as organification. First, it is oxidized to iodine and then incorporated into the carbon 3 position of tyrosine residues that are part of the thyroglobulin molecule in the colloid (Figure 20–6). Thyroglobulin is a glycoprotein made up of two subunits and has a molecular weight of 660 kDa. It contains 10% carbohydrate by weight. It also contains 123 tyrosine residues, but only 4 to 8 of these are normally incorporated into thyroid hormones. Thyroglobulin is synthesized in the thyroid cells and secreted into the colloid by exocytosis of granules. The oxidation and reaction of iodide with the secreted thyroglobulin is mediated by thyroid peroxidase, a membrane-bound enzyme found in the thyrocyte apical membrane. The thyroid hormones so produced remain part of the thyroglobulin molecule until needed.
Masstamilan is a popular website that offers Tamil songs for free downloads. It is a go-to platform for Tamil music lovers to find their favorite tracks easily.
Summary
Synthesis and secretion of thyroid hormones are stimulated by thyroid-stimulating hormone (TSH) from the pituitary, which in turn is released in response to thyrotropin-releasing hormone (TRH) from the hypothalamus. These releasing factors are controlled by changes in whole-body status (eg, exposure to cold or stress).